Our Services
Root Canal Cost in Vietnam 2026: From $80–$250 | Picasso Dental Clinic
How much is a root canal in Vietnam? From $80–$250 vs $700–$1,500 in the US. 95%+ success rate, ADA-standard endodontic care. Free quote before you fly.
Last updated: May 29, 2026
What Is Root Canal Treatment?
Root canal treatment is an endodontic procedure that saves a natural tooth whose internal pulp tissue has become infected or irreversibly inflamed. Without treatment, the infection can progress through the five stages of tooth decay and eventually require tooth extraction. The dental pulp, a soft tissue containing nerves, blood vessels, and connective tissue, sits inside the tooth’s pulp chamber and root canals. When bacteria penetrate the pulp through deep decay, cracks, or trauma, infection develops and can cause severe pain, abscess formation, and bone loss. According to the American Association of Endodontists, root canal treatment has a success rate exceeding 95 percent when performed with modern techniques and proper restoration. During the procedure, the infected pulp is removed, the canal system is cleaned, shaped, and disinfected, and the space is sealed with biocompatible material. At Picasso Dental Clinic in Hanoi, Vietnam, root canal treatment is performed using advanced rotary instruments and digital imaging to ensure thorough, predictable results.
Who Needs Root Canal Treatment?
Learn to recognise the 7 warning signs that indicate root canal treatment before the infection spreads.
Root canal treatment may be necessary if you experience any of the following:
- Severe, persistent toothache that worsens when chewing or applying pressure
- Prolonged sensitivity to hot or cold temperatures that lingers after the stimulus is removed
- Darkening or discoloration of a tooth compared to adjacent teeth
- Swelling, tenderness, or a recurring pimple on the gum near a painful tooth
- Deep decay visible on X-rays that has reached or approached the nerve
- A cracked or fractured tooth with pulp exposure
- Trauma to a tooth that has caused pulp damage even without visible decay
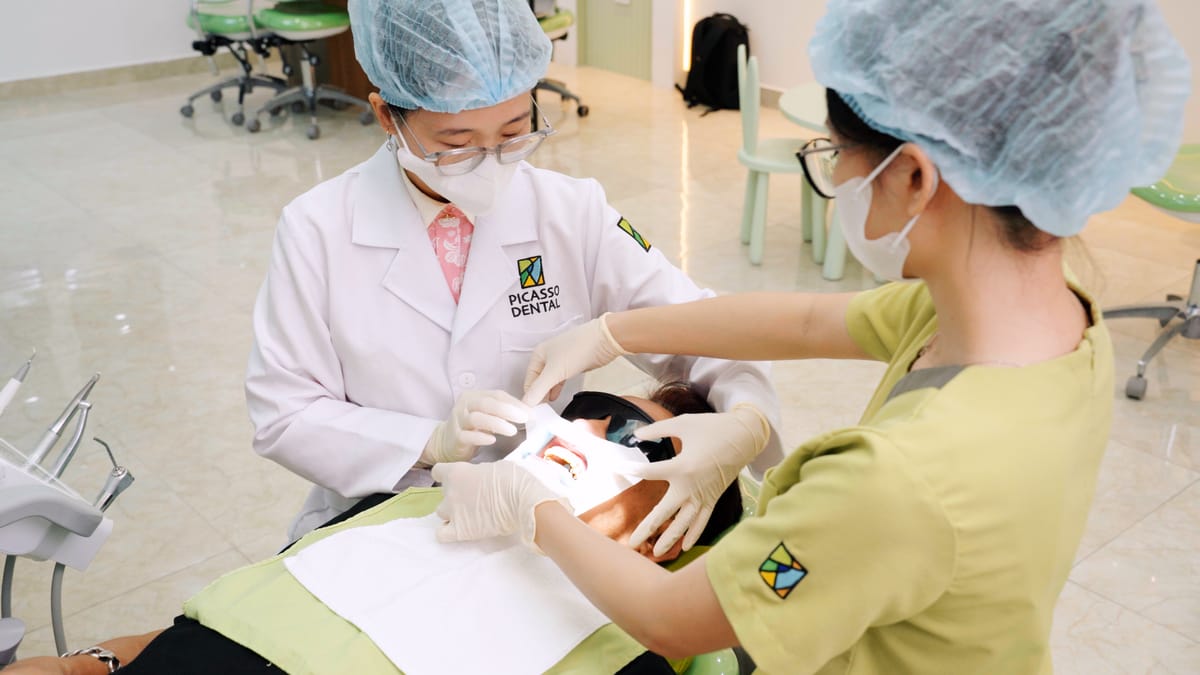
The Root Canal Treatment Process at Our Hanoi Clinic
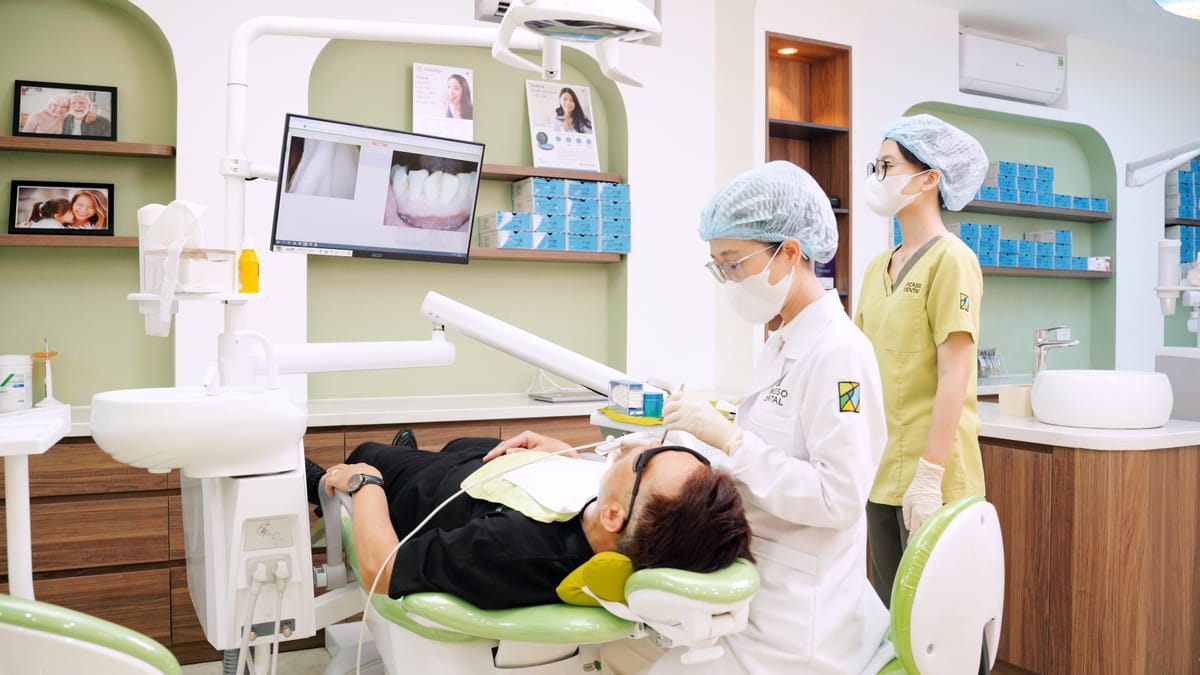
Step 1: Diagnosis and Digital Imaging
Your dentist at Picasso Dental Clinic examines the tooth and takes digital X-rays to evaluate the extent of infection, the number and shape of root canals, and the condition of surrounding bone. This precise imaging guides the entire treatment plan.
Step 2: Anesthesia and Tooth Isolation
Local anesthesia is administered to numb the tooth and surrounding tissues completely. A rubber dam is placed around the tooth to isolate it from saliva and maintain a sterile working field throughout the procedure.
Step 3: Pulp Removal, Cleaning, and Shaping
An access opening is made through the crown of the tooth. Using rotary endodontic instruments, the infected or inflamed pulp is removed from the pulp chamber and each root canal. The canals are carefully shaped and irrigated with antimicrobial solutions such as sodium hypochlorite to eliminate bacteria and debris.
Step 4: Canal Filling and Sealing
The cleaned and shaped canals are filled with gutta-percha, a biocompatible thermoplastic material, and sealed with adhesive cement to prevent bacterial re-entry and reinfection.
Step 5: Crown Restoration
A temporary filling is placed initially. Within two to four weeks, a permanent dental crown is fabricated and cemented over the treated tooth to restore its full strength, function, and appearance.
Benefits of Root Canal Treatment
- Saves the natural tooth – avoids extraction and the subsequent need for an implant, bridge, or denture
- Eliminates infection and pain – removes the bacterial source of toothache, abscess, and swelling
- Restores full chewing function – the crowned tooth functions like any other natural tooth
- Over 95 percent success rate – one of the most predictable procedures in dentistry according to the American Association of Endodontists
- Cost-effective long-term solution – preserving a natural tooth is less expensive than extraction followed by implant replacement
- Prevents bone loss – keeping the natural tooth root in place maintains jawbone volume and density
- Completed in one to two visits – most root canals at Picasso Dental Clinic in Hanoi are finished in a single appointment
Root Canal Treatment Cost in Vietnam Compared to Other Countries
| Country | Root Canal Treatment Cost (USD) |
|---|---|
| Vietnam (Hanoi) | $80 – $200 |
| United States | $700 – $1,500 |
| United Kingdom | $400 – $1,000 |
| Australia | $600 – $1,200 |
Prices reflect typical ranges for anterior and molar root canal treatment without crown. Costs vary by tooth location, number of canals, and case complexity. Vietnam pricing is based on current rates at internationally accredited dental clinics in Hanoi. International pricing sourced from national dental association fee surveys and dental tourism comparison databases.
Aftercare and Recovery
After root canal treatment at Picasso Dental Clinic in Hanoi, follow these guidelines for optimal healing:
- Avoid chewing on the treated side until the permanent crown is placed
- Take prescribed antibiotics and pain medication as directed by your dentist
- Mild soreness or tenderness around the treated tooth is normal for two to three days
- Use over-the-counter anti-inflammatory medication such as ibuprofen if needed for discomfort
- Brush and floss normally but be gentle around the treated tooth
- Avoid biting into very hard foods with the treated tooth until the crown is placed
- Attend your follow-up appointment for crown placement within two to four weeks
- Once the permanent crown is placed, care for the tooth as you would any natural tooth
- Schedule regular dental checkups every six months to monitor the treated tooth
Why Choose Picasso Dental Clinic in Hanoi for Root Canal Treatment?
Picasso Dental Clinic is located at 16 Chau Long, Ba Dinh District, Hanoi, Vietnam, in the heart of the city near the Old Quarter and West Lake. With 6 clinic locations across Vietnam, Picasso Dental has served over 70,000 patients and maintains a 4.9 out of 5 rating based on 3,921 verified patient reviews.
Our root canal treatments are performed by experienced endodontists using rotary nickel-titanium instruments, electronic apex locators, and digital radiography for precise canal preparation and thorough disinfection. All procedures follow ADA and WHO sterilization and infection control protocols.
Our English-speaking dental team provides clear communication, detailed treatment explanations, and transparent pricing for international patients, expatriates, and dental tourists visiting Hanoi. Whether you are based in the Old Quarter, West Lake, or anywhere in Hanoi, Picasso Dental Clinic offers accessible, world-class endodontic care at a fraction of Western prices.
Medically reviewed by Dr. Emily Nguyen, Principal Dentist at Picasso Dental Clinic, Hanoi, Vietnam. Last updated: March 2026.
Frequently Asked Questions About Root Canal Treatment in Hanoi
Is root canal treatment painful in Hanoi?
Root canal treatment at Picasso Dental Clinic in Hanoi is performed under effective local anesthesia and is generally no more uncomfortable than receiving a standard filling. Most patients report immediate relief from their toothache once the infected pulp is removed.
How long does a root canal take at Picasso Dental Clinic?
A root canal on a single-canal front tooth typically takes 45 to 60 minutes. Molars with three or four canals may require 60 to 90 minutes. Most treatments at our Hanoi clinic are completed in one appointment.
What happens if I do not get a root canal?
Without treatment, the infection spreads deeper into the jawbone, potentially forming an abscess, destroying surrounding bone, and eventually requiring tooth extraction. In rare cases, untreated dental infections can lead to serious systemic complications.
Do I need a crown after root canal treatment?
Yes, a dental crown is strongly recommended after root canal treatment. The treated tooth becomes more brittle because the pulp that supplied moisture and nutrients has been removed. A crown restores strength and protects the tooth from fracture.
How long does a root-canal-treated tooth last?
With a properly fitted crown and consistent oral hygiene, a root-canal-treated tooth can last a lifetime. Regular dental checkups at Picasso Dental Clinic help monitor the tooth and ensure long-term success.
How much does root canal treatment cost in Hanoi, Vietnam?
Root canal treatment at Picasso Dental Clinic in Hanoi costs between 80 and 200 USD depending on the tooth location and number of canals. This is significantly lower than the 700 to 1,500 USD typically charged in the United States.
Can I travel after root canal treatment in Hanoi?
Most patients can fly within 24 to 48 hours after root canal treatment. Avoid flying immediately after the procedure if you experience significant swelling. Your dentist at Picasso Dental Clinic will advise you based on your specific case.
What is the success rate of root canal treatment?
According to the American Association of Endodontists, root canal treatment has a success rate exceeding 95 percent when performed with modern techniques and followed by proper restoration with a crown.
How do I know if I need a root canal?
Common signs include severe persistent toothache, prolonged sensitivity to hot or cold, darkening of the tooth, swelling or tenderness in nearby gums, and a pimple-like bump on the gum near the affected tooth. A dental examination with X-rays confirms the diagnosis.
Is root canal treatment safe for international patients visiting Hanoi?
Yes. Picasso Dental Clinic follows ADA and WHO sterilization and treatment protocols. Our English-speaking dentists use digital imaging and rotary endodontic instruments to deliver safe, predictable root canal outcomes for international patients.
Can a root canal fail?
Root canal failure is uncommon but can occur if bacteria persist in accessory canals, the tooth develops a new crack, or the restoration is delayed. Retreatment or apicoectomy can address failed root canals. Timely crown placement significantly reduces failure risk.
What anesthesia is used for root canal treatment in Vietnam?
Local anesthesia is the standard for root canal treatment at Picasso Dental Clinic. The tooth and surrounding tissues are completely numbed before any work begins. Sedation options are available for patients with dental anxiety.
Related Reading
- 6 Steps of Root Canal Treatment Procedure — A detailed walkthrough of each stage of root canal therapy from diagnosis to crown placement
- Do You Always Need a Crown After a Root Canal? — When crowns are essential and when alternative restorations may be appropriate
- Root Canal Treatment vs Tooth Extraction — Compare the long-term costs, recovery, and outcomes of both options
- What Are the Side Effects of Root Canal Treatment? — Common post-treatment symptoms and how to manage them
- Broken File in Root Canal During Treatment — What happens when an instrument fragment remains and how it is managed
- Pain-Free Dentistry with Local Anesthesia — How modern anesthesia makes dental procedures comfortable
- Dental Crown Services — Explore crown options for protecting your root canal treated tooth
- Dental Costs in Vietnam — Compare treatment pricing across countries
Free Consultation
Get your quote in 2 hours
Leave your details and a coordinator will reply with a personalised treatment plan and itemised quote during business hours.
Request received.
Thank you. We'll be in touch within 2 hours with your personalised plan and quote.
Real Patients, Real Results
Smile Transformations
Every case below was completed at Picasso Dental Clinic. Each photo shows the same patient before and after their treatment.
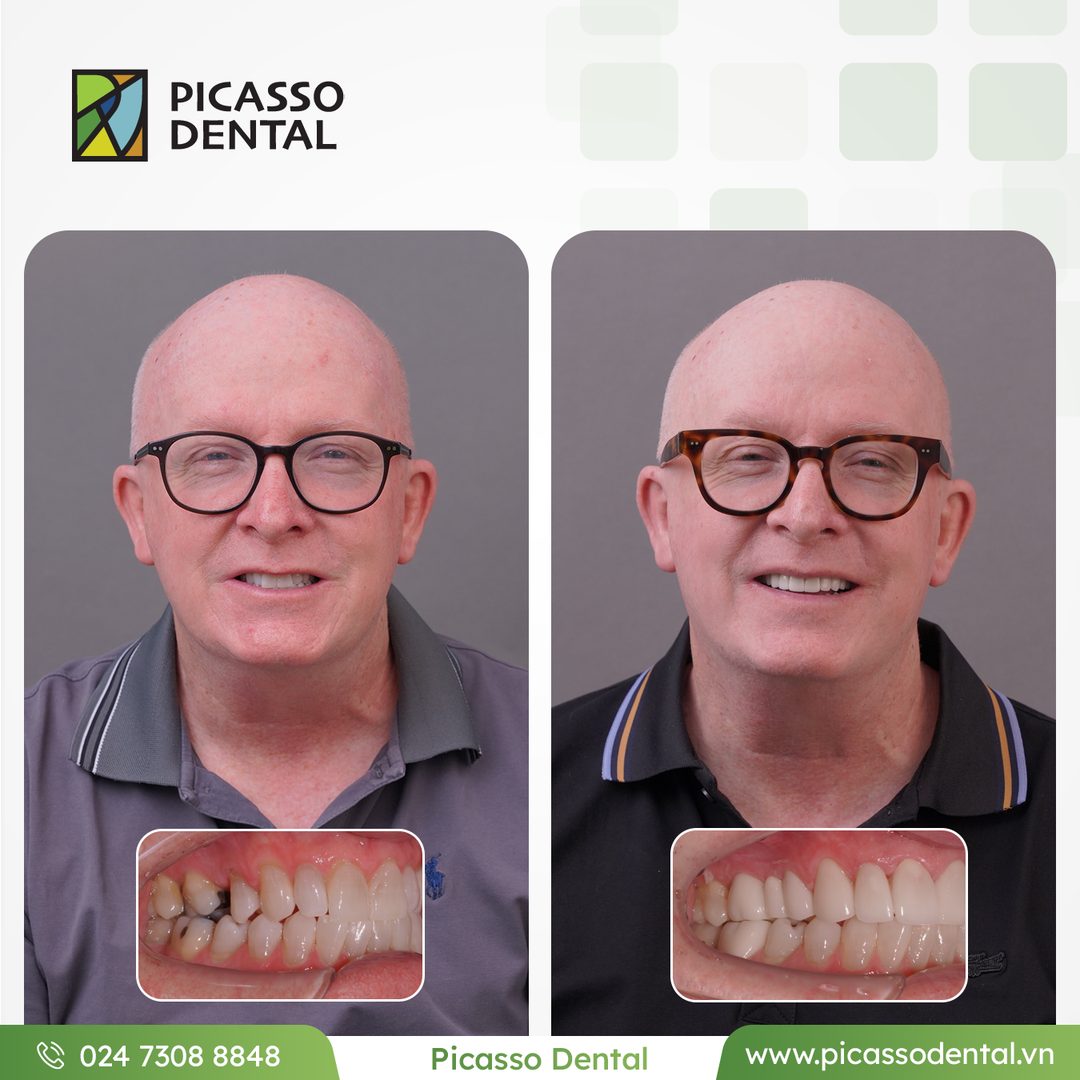
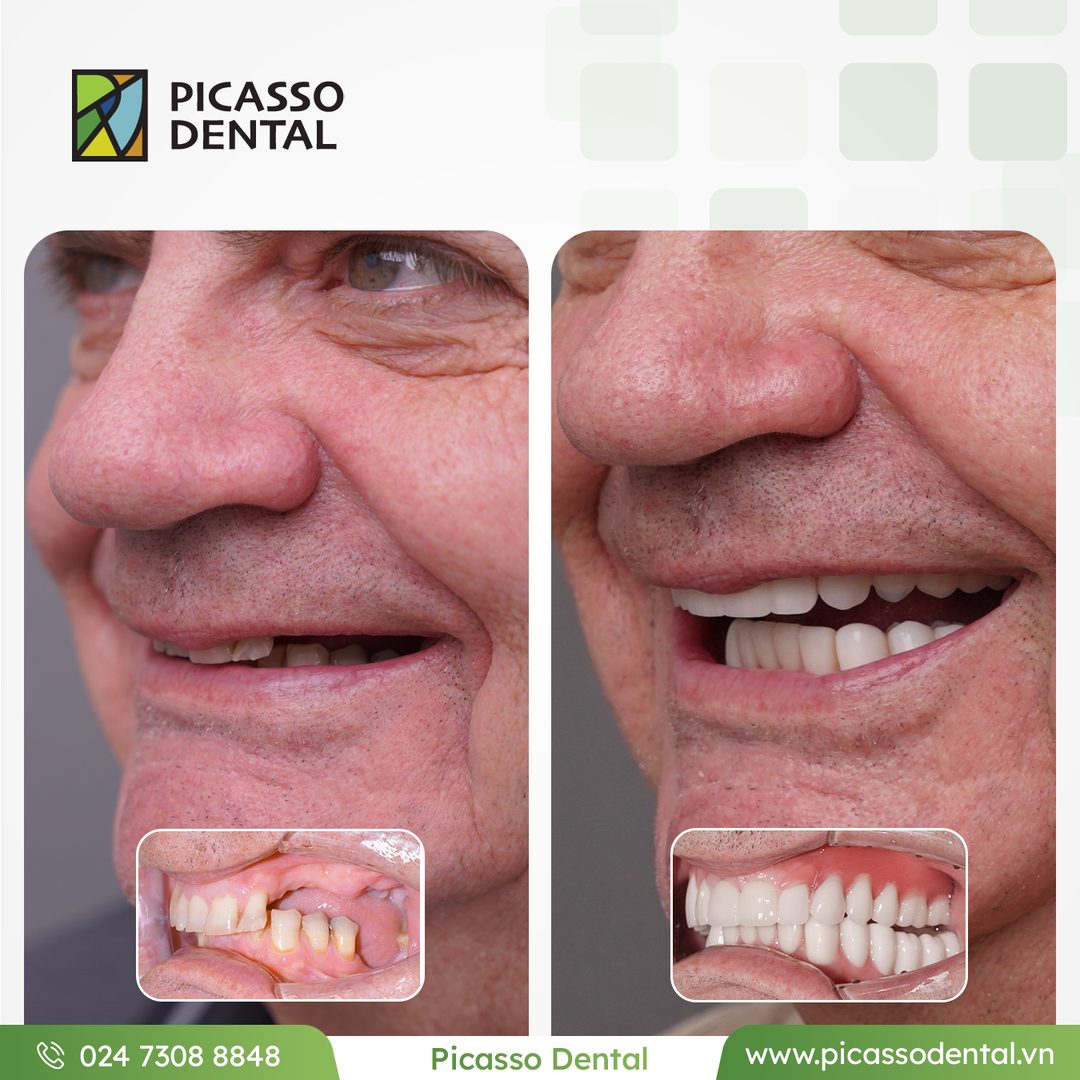

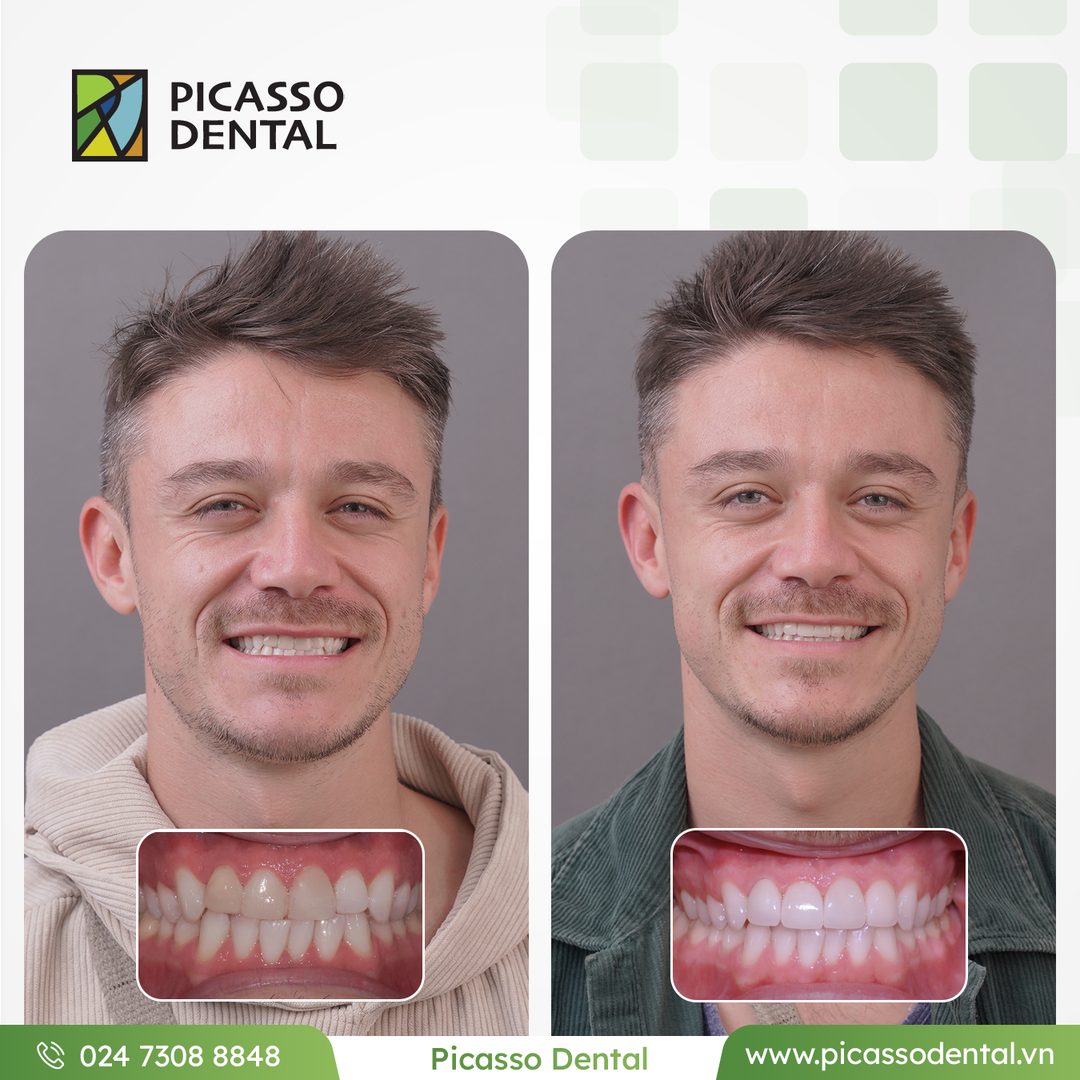

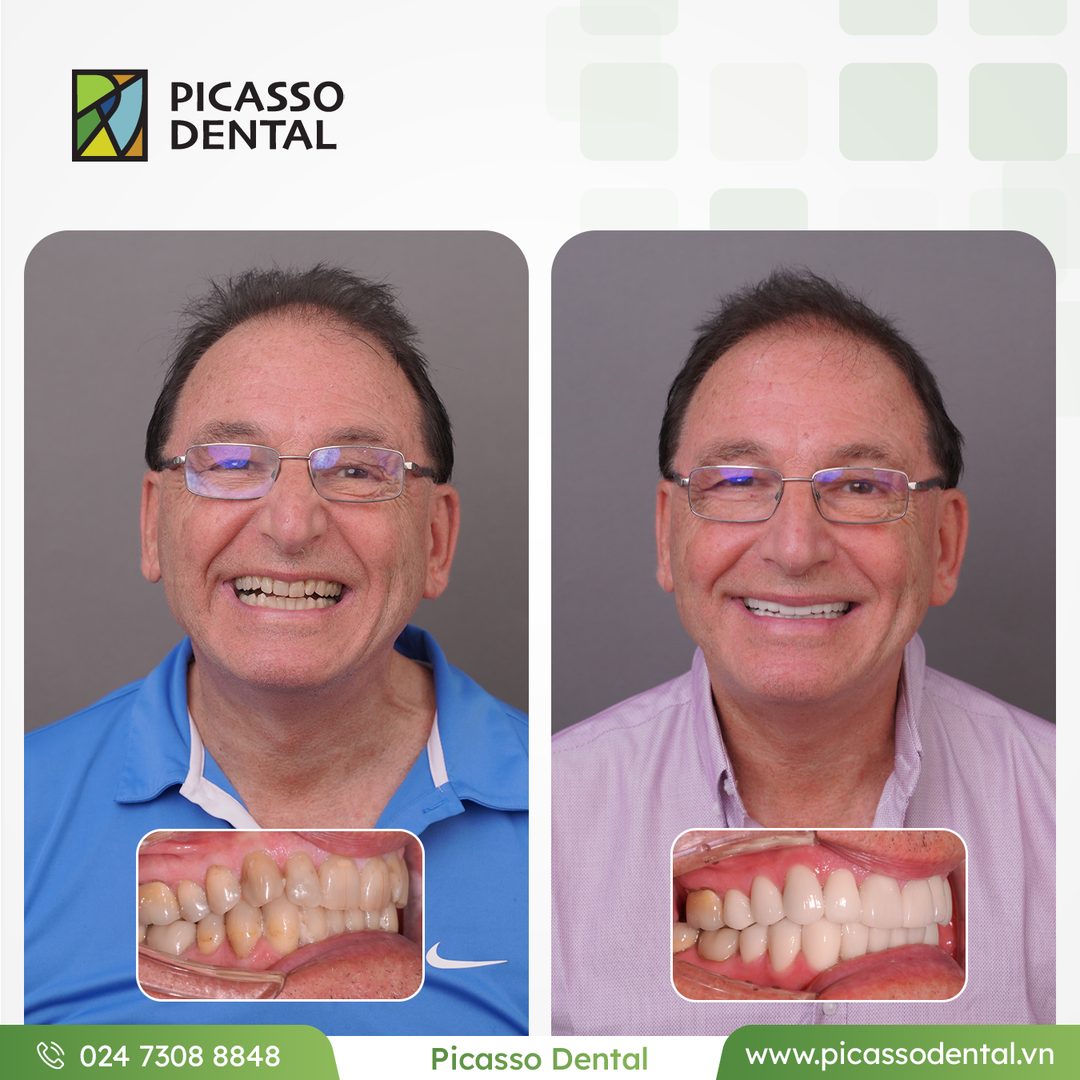
Photos used with patient consent. Individual results vary.
View more transformations arrow_forwardReady to Get Started?
Contact Picasso Dental Clinic to discuss your treatment options and schedule a free consultation.
"The dentists were amazing and explained everything in near-perfect English. The staff were warm and welcoming from the minute I walked inside."
— Keith S., Australia
via WhatClinic
"The dentist was thorough, kind, and explained everything clearly. Had X-rays, fillings, and whitening done with excellent results."
— Thomas Wallace
via Google
Video Testimonials
Hear Directly from Our Patients
Real patients share their experiences at Picasso Dental Clinic in their own words.
Other Services
All-on-4 Dental Implants — Where to Get Them, Cost from $4,500/Arch | Hanoi · Da Nang · HCMC
All-on-4 dental implants from $4,500/arch (vs $15,000–$25,000 in Australia, $20,000+ in the US). Same-day fixed teeth, 94.8% 10-year survival. Find an All-on-4 dental implants clinic near you — 6 locations in Vietnam: Hanoi (2), Da Nang (2), Ho Chi Minh City, Da Lat. Straumann, Nobel Biocare, Osstem. Free quote.

Cosmetic Dentistry Vietnam 2026 — Veneers $250, Whitening $150, Smile Makeover $1,500+
Cosmetic dentistry in Vietnam at Picasso Dental Clinic: porcelain veneers from $250/tooth, Zoom whitening from $150, composite bonding from $80, full smile makeovers from $1,500. Save 50–70% vs the US, UK & Australia. Free digital smile design consultation.
Dental Implants in Vietnam 2026: From $800 — Cost, Brands & What to Expect
Dental implant cost in Vietnam: Straumann, Nobel Biocare & Osstem from $800/implant vs $3,000–$5,000 in the US. 96.4% success rate, 4.9/5 · 3,900+ reviews. Free quote.
Root Canal Cost in Vietnam 2026: From $80–$250 | Picasso Dental Clinic
Get a free consultation at Picasso Dental Clinic.
